Daily Habits That Help You Breathe Easier with COPD
Living with Chronic Obstructive Pulmonary Disease (COPD) presents daily challenges, but adopting targeted habits can significantly improve breathing comfort and lung function. Small, consistent changes in daily routines create meaningful differences in respiratory health and overall well-being for people managing this progressive condition.
Practice Controlled Breathing Techniques
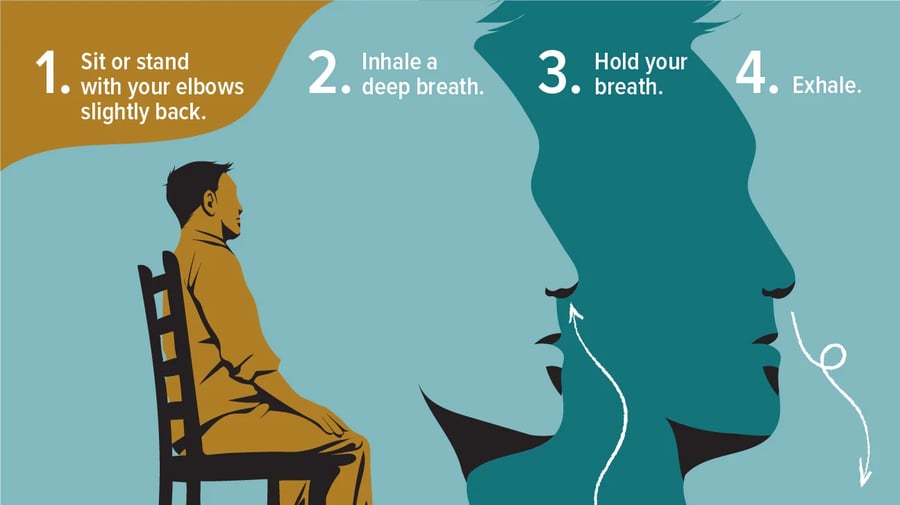
Pursed-lip breathing and diaphragmatic breathing are two fundamental techniques that help strengthen respiratory muscles and improve oxygen exchange. Pursed-lip breathing involves inhaling slowly through the nose for two counts, then exhaling through pursed lips for four counts, which keeps airways open longer and reduces trapped air in the lungs. Diaphragmatic breathing engages the diaphragm rather than chest muscles, allowing deeper breaths with less effort and reducing the work of breathing by up to 50 percent in some individuals.
Practicing these techniques for just 5-10 minutes three times daily helps retrain breathing patterns and builds muscle memory. Many pulmonary rehabilitation programs teach these methods as foundational skills because they provide immediate relief during shortness of breath episodes and improve exercise tolerance over time. The National Heart, Lung, and Blood Institute recommends incorporating breathing exercises into daily routines as part of comprehensive COPD management.
Maintain Regular Physical Activity
Exercise may seem counterintuitive when breathing is difficult, but regular physical activity is one of the most effective ways to improve lung function and reduce COPD symptoms. Low-impact activities such as walking, swimming, or stationary cycling strengthen the heart and muscles, making the body more efficient at using oxygen. Starting with just 10-15 minutes of gentle movement daily and gradually increasing duration builds endurance without overwhelming the respiratory system.
Pulmonary rehabilitation programs combine supervised exercise with education and support, helping individuals safely increase activity levels. These programs have been shown to reduce hospitalizations, improve exercise capacity, and enhance quality of life for people with moderate to severe COPD. Even simple activities like gardening, stretching, or light household tasks contribute to maintaining muscle strength and preventing the deconditioning that worsens breathlessness.
Optimize Indoor Air Quality
The air quality inside living spaces directly impacts respiratory comfort and symptom severity. Removing irritants such as dust, mold, pet dander, and chemical fumes reduces inflammation and airway irritation. Using HEPA filters in heating and cooling systems traps airborne particles, while running air purifiers in frequently used rooms provides additional protection against pollutants and allergens.
Avoiding household products with strong fragrances or harsh chemicals prevents respiratory irritation. Switching to fragrance-free cleaning supplies, avoiding aerosol sprays, and ensuring proper ventilation when cooking or using any cleaning products minimizes exposure to triggers. Maintaining indoor humidity levels between 30-50 percent prevents both dryness that irritates airways and excess moisture that promotes mold growth. Simple tools like hygrometers measure humidity, and dehumidifiers or humidifiers adjust levels as needed.
Follow Medication Schedules Consistently
Adhering to prescribed medication regimens is critical for controlling COPD symptoms and preventing exacerbations. Bronchodilators open airways and make breathing easier, while inhaled corticosteroids reduce inflammation in the lungs. Taking medications exactly as prescribed—at the correct times and with proper inhaler technique—ensures maximum therapeutic benefit and helps maintain stable lung function.
Many people struggle with inhaler technique, which reduces medication effectiveness by up to 70 percent when done incorrectly. Scheduling regular reviews with healthcare providers or respiratory therapists to verify proper technique ensures medications reach deep into the lungs where they work best. Setting daily reminders on phones or using pill organizers helps maintain consistency, especially when managing multiple medications with different dosing schedules.
Prioritize Nutrition and Hydration
Proper nutrition supports lung health and provides energy needed for breathing, which burns significantly more calories in people with COPD than in those with healthy lungs. Eating smaller, more frequent meals throughout the day prevents the feeling of fullness that can press against the diaphragm and make breathing more difficult. Choosing nutrient-dense foods rich in protein, healthy fats, and complex carbohydrates helps maintain muscle mass and energy levels.
Staying well-hydrated keeps mucus thin and easier to clear from airways, reducing the risk of infections. Drinking six to eight glasses of water daily—unless otherwise directed by a healthcare provider—supports respiratory function and overall health. Some individuals with COPD benefit from limiting sodium intake to reduce fluid retention, while others may need additional calories to prevent weight loss. Consulting with a registered dietitian who specializes in pulmonary conditions can provide personalized nutrition strategies tailored to individual needs and symptoms.
Prevent Respiratory Infections
Respiratory infections are the leading cause of COPD exacerbations, which can cause lasting damage to lung function. Practicing diligent hand hygiene by washing hands frequently with soap and water for at least 20 seconds reduces exposure to viruses and bacteria. Avoiding crowded spaces during flu season and maintaining distance from people who are sick provides additional protection against infections.
Staying current with vaccinations is one of the most effective preventive measures available. The Centers for Disease Control and Prevention recommends annual influenza vaccines and pneumococcal vaccines for all adults with COPD, as these significantly reduce the risk of serious complications from respiratory infections. Newer vaccines, including those for COVID-19 and RSV, offer additional protection and should be discussed with healthcare providers to determine appropriate timing and recommendations.
Create a Smoke-Free Environment
Eliminating all tobacco smoke exposure is the single most important action anyone with COPD can take to slow disease progression. Continuing to smoke accelerates lung damage and reduces the effectiveness of medications and other treatments. Quitting smoking at any stage of COPD provides benefits, including reduced symptom severity, fewer exacerbations, and improved survival rates.
Avoiding secondhand smoke is equally important, as even brief exposure causes immediate airway irritation and inflammation. Creating smoke-free zones in homes and vehicles protects lung health and reduces symptom flare-ups. Many resources support smoking cessation, including nicotine replacement therapies, prescription medications, counseling services, and support groups. Healthcare providers can recommend appropriate cessation strategies and connect individuals with free resources and support programs designed to increase success rates.
Monitor Symptoms and Seek Early Intervention
Developing awareness of personal symptom patterns enables early recognition of exacerbations, when prompt treatment can prevent serious complications. Keeping a daily log of symptoms such as increased breathlessness, changes in mucus color or amount, chest tightness, or reduced exercise tolerance helps identify trends and triggers. Many people use simple tracking apps or journals to record symptoms, medication use, and activity levels.
Understanding when to contact healthcare providers prevents delays in treatment that can lead to hospitalizations. Warning signs requiring immediate medical attention include severe shortness of breath at rest, confusion, chest pain, bluish lips or fingernails, or symptoms not relieved by usual medications. Having an action plan developed with a healthcare provider that outlines specific steps to take when symptoms worsen provides confidence and clear guidance during concerning episodes.
Build a Support Network
Connecting with others who understand the challenges of living with COPD reduces feelings of isolation and provides practical strategies for managing daily life. Support groups—whether in-person or online—offer opportunities to share experiences, learn coping techniques, and find encouragement from people facing similar situations. Many hospitals, community centers, and patient advocacy organizations facilitate regular meetings and online forums.
Engaging family members and friends in care planning ensures adequate support during difficult times and helps loved ones understand the condition. Educating those in close contact about COPD symptoms, triggers, and management strategies enables them to provide appropriate assistance and recognize when additional help is needed. Pulmonary rehabilitation programs often include education sessions for family members, creating a shared understanding of the condition and treatment goals.